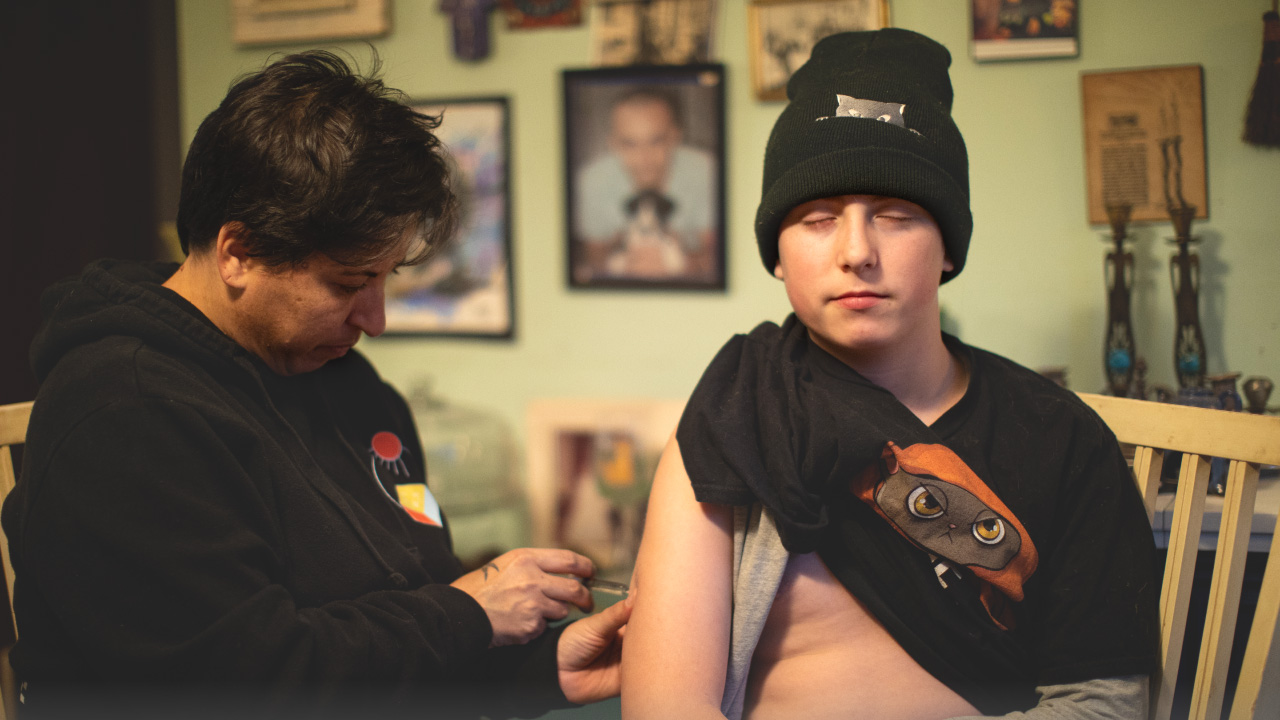
Fort Worth, TX
This individual is providing context about their experience living with HAE and is not commenting about an investigational therapy from Intellia Therapeutics.
“When I finally learned I had HAE, there was a moment of elation, and then right after that, it was, ‘Oh my gosh, I have this. And it’s forever.’”
Kim’s journey with the rare genetic disease hereditary angioedema (HAE) began long before she knew its name.
For much of her childhood, she was “the kid who was always sick” – a challenging burden for a child to carry. She missed weeks of school due to unexplained swelling and abdominal pain that no doctors – from pediatricians and GI specialists to surgeons and chiropractors – could explain.
At one point, her mother even brought her to a psychiatrist. She didn’t think her daughter’s mental health was the explanation, but the family was desperate to help her. Kim left that visit with a prescription for an anxiety medication.
The turning point in Kim’s journey to a diagnosis came when she was in her 30s. She had a laryngeal swell – a terrifying and potentially life-threatening symptom that Benadryl failed to help – and went to the emergency room with her husband.

Kim and her husband, Brent
But the laryngeal swells kept recurring.
Over the course of two weeks, Kim visited the ER three times. Each visit ended the same way: temporary relief but no answers.
“They gave me Benadryl, watched me for a while, and sent me home,” she says. “By the third time, one of the doctors finally said, ‘It’s some sort of angioedema – but I don’t know what’s causing it.’”
That word – angioedema – was the clue Kim had been waiting for. Determined to understand what was happening to her body, she began researching on her own. One evening, she found information about hereditary angioedema, a rare genetic condition that seemed to fit everything she’d experienced. She also discovered that a nearby physician was conducting a clinical trial in HAE.
“I picked up the phone and called,” she says. “The nurse told me I probably didn’t have it, but I insisted on being tested.”
Two weeks later, the results came back: positive. Kim finally had an answer.
“It was the weirdest mix of emotions,” she remembers. “It was this moment of, I have an answer. And then right after that, Oh my gosh, I have an answer – and it’s a rare disease with no cure.”
By then, years of uncontrolled attacks had taken a toll. “I was really sick at that time,” she recalls. “I ended up going on disability for two years because I was having so many laryngeal and abdominal swells back-to-back. It was just constant.”
Still, the diagnosis marked a turning point. After decades of uncertainty, Kim finally had a name for what she was living with.
Getting a diagnosis didn’t mean the end of Kim’s struggles, however. It simply changed the nature of them. The physical danger of the unknown shifted into the emotional weight of living with an incurable lifelong condition.
“Once I finally got a diagnosis, the emotional toll shifted,” she explains. “It becomes more about the unpredictable nature of HAE. Am I going to be able to do things with my family? Am I going to be the one constantly disrupting plans because I’m still having breakthrough attacks?”

Kim’s son, Trevor, and her husband, Brent
The stories she tells paint a picture of how HAE affects every corner of life. She recalls an attack on a cruise ship in Alaska that forced her family to miss an excursion, and another on a beach in Hawaii that left her watching from the sidelines. “It impacts everything,” she says.
Beyond the physical burden, HAE carries a financial and psychological toll, involving constant negotiations with insurance, fear of medication shortages, and the ever-present worry of when the next attack will strike.
“It’s a terrible thing to have because you just don’t know when it’s going to hit, or how it’s going to hit,” Kim says. “The fear is always there—a tickle in your throat, and you think, ‘Do I have a cold, or is this a swell?’”
Today, Kim’s condition is more stable, but she remains vigilant. She’s been on eight different treatments and has learned to advocate for her needs at every step.
“I’m still having attacks. It’s not gone,” she says. “And so my pie in the sky hope is that we get to the point where we don’t have attacks, we don’t have to worry about attacks, you don’t have to be worried about the logistics of, oh my gosh, I just got denied again from the insurance company.”
Through every stage of her journey, Kim’s family has been her anchor – from her parents’ relentless search for answers when she was young to the unwavering understanding of her husband and son today. They adjust plans, offer support during attacks, and remind her that she isn’t facing HAE alone. Whether it’s staying behind with her when she can’t participate in an activity or making sure she has her medications close at hand, she says their patience and love have helped her live more confidently with a disease that is terribly unpredictable.
To Kim’s surprise – and relief – no one else in her family has been diagnosed with hereditary angioedema. Her son was tested twice, once as a child and again more recently with advanced diagnostics. “I finally feel confident saying he doesn’t have it,” Kim notes, “and that means he can’t pass it on to his future children.”

Kim, and her son, Trevor
Above all, Kim hopes her story helps others with HAE feel more understood.
“I want people to know they’re not alone,” she says. “You can still have a full life with HAE — but it’s also okay for us to want more.”

USHAE- 250010 v1.0 Dec 2025