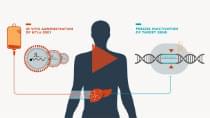
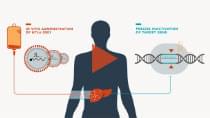
We are focused on revolutionizing medicine by developing product candidates for a range of severe diseases leveraging CRISPR expertise and other core technologies and therapeutic approaches.
Indication
Preclinical
Clinical
Clinical
Submission
Clinical
Clinical
Preclinical
- Lead refers to lead development and commercial party.
1. Lonvo-z (lonvoguran ziclumeran), formerly referred to as NTLA-2002. 2. Nex-z (nexiguran ziclumeran), formerly referred to as NTLA-2001; Regeneron shares 25% of worldwide development costs and commercial profits for the ATTR program and has an option to enter into a co-promotion agreement for the U.S. commercialization. 3. Hemophilia B is being advanced solely by Regeneron; Intellia is eligible for milestones and royalties. 4. AVC-201 and AVC-203 are wholly owned by AvenCell and utilize proprietary allogeneic cell engineering technology licensed from Intellia. 5. Intellia is advancing both wholly owned and partnered programs.
Download